Cortisol and Belly Fat Explained: Why Stress Targets Your Waist
Key Takeaways:
- Counter-Intuitive Insight: Visceral fat (belly fat) is not just stored energy; it is an active endocrine organ that secretes its own inflammatory hormones and cortisol, creating a self-perpetuating cycle.
- Specific Number: Abdominal fat cells have up to 4 times more cortisol receptors than fat cells in other parts of the body, making them magnets for stress-induced storage.
- Simple Habit: Doing 10 minutes of “optical flow” (walking while looking forward) after a stressful event can manually lower cortisol levels.
- Realistic Expectation: You cannot “crunch” away hormonal belly fat; lowering the stress hormone baseline is the only way to signal the body to release these specific stores.
For many people, the struggle with weight is not about a lack of discipline or excessive calories. It is about a biological signal that screams “danger.” You might be eating clean and exercising daily, yet the “spare tire” around your midsection refuses to budge. This frustration is often the result of a misunderstood hormonal mechanism. Having the relationship between cortisol and belly fat explained through a biological lens changes the strategy entirely.
In a healthy system, cortisol is a superhero hormone. It wakes you up in the morning, reduces inflammation, and provides fuel during acute stress. However, modern life has trapped us in a state of chronic, low-grade emergency. When cortisol remains elevated, the body shifts into a survival mode that prioritizes fat storage in the abdominal cavity.
Much of this chronic stress is driven by constant digital stimulation, which is why learning how to simplify digital life is often the first step in lowering baseline cortisol.
Hormonal stress responses like cortisol have been extensively studied by the Society for Endocrinology, particularly for their role in metabolism and abdominal fat storage.
This guide will move beyond the “calories in, calories out” model. We will explore the specific receptor sites in your abdomen, the connection between stress and insulin, and the actionable, science-backed steps to convince your nervous system that it is safe to burn fat again.
This guide is for people who are doing “everything right” eating reasonably well, exercising, and still struggling with stubborn belly fat, fatigue, or anxiety. It is especially relevant if you feel wired but tired, crave sugar under stress, or notice your weight fluctuates with sleep quality.
This guide is not for those seeking rapid weight loss through extreme dieting or excessive cardio. Cortisol-driven fat storage requires calming the nervous system, not punishing the body.
1. What Is the Biological Link Between Stress and Fat?
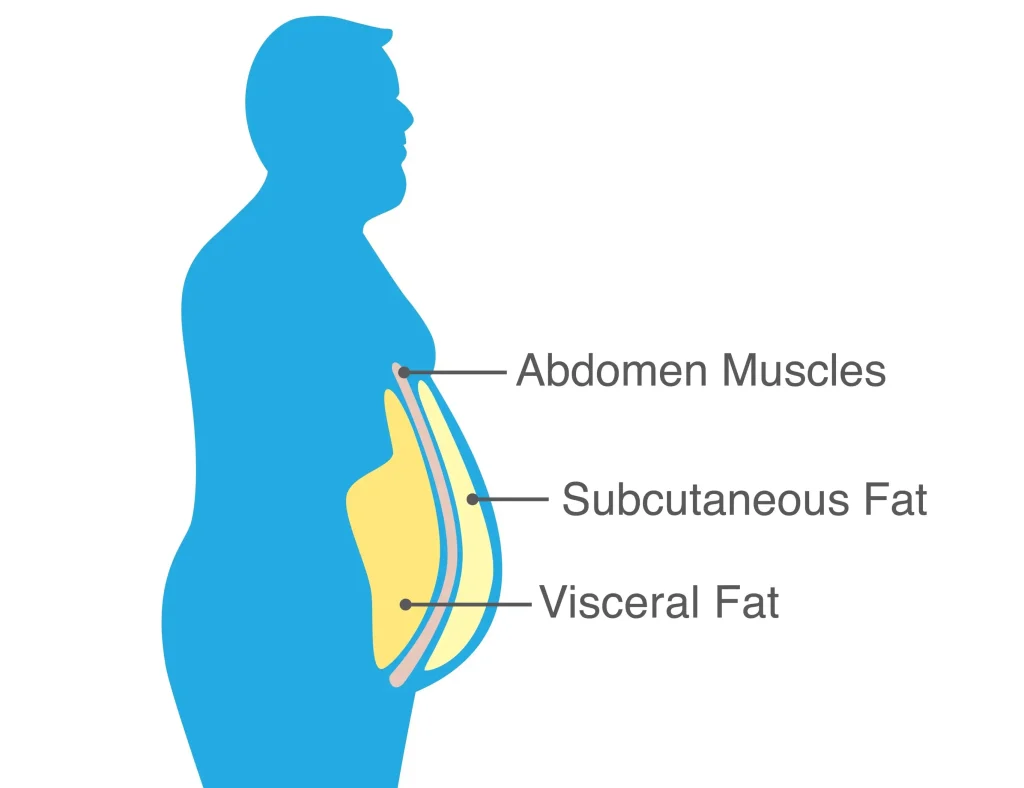
The link between cortisol and belly fat centers on the HPA Axis (Hypothalamus-Pituitary-Adrenal). When the brain perceives constant stress, it triggers the release of cortisol, which mobilizes glucose for energy. If this energy is not used (i.e., you are sitting at a desk, not running from a tiger), the body redeposits this excess energy as visceral fat deep abdominal fat that surrounds vital organs.
The HPA Axis Function
The HPA axis is your body’s central stress response system. It acts as a feedback loop between the brain and the adrenal glands.
- The Alarm Signal: When you feel stressed, the hypothalamus signals the pituitary gland, which then tells the adrenal glands to release cortisol.
- Mobilization: Cortisol’s primary job is to flood the bloodstream with glucose (sugar) so you have the fuel to fight or flee.
- The Mismatch: In modern life, our stress is psychological (emails, traffic), not physical. We do not burn off this glucose spike, so the body must store it again.
- Storage Signal: Because the body thinks it is in a harsh environment, it stores this energy in the most easily accessible place for the liver: the abdomen.
Clinical explanations from the Cleveland Clinic show how chronic stress disrupts the HPA axis and drives hormonal weight gain.
Visceral Fat as an Active Organ
We used to think fat was just passive storage. We now know that visceral fat (the kind behind the abdominal wall) is biologically active.
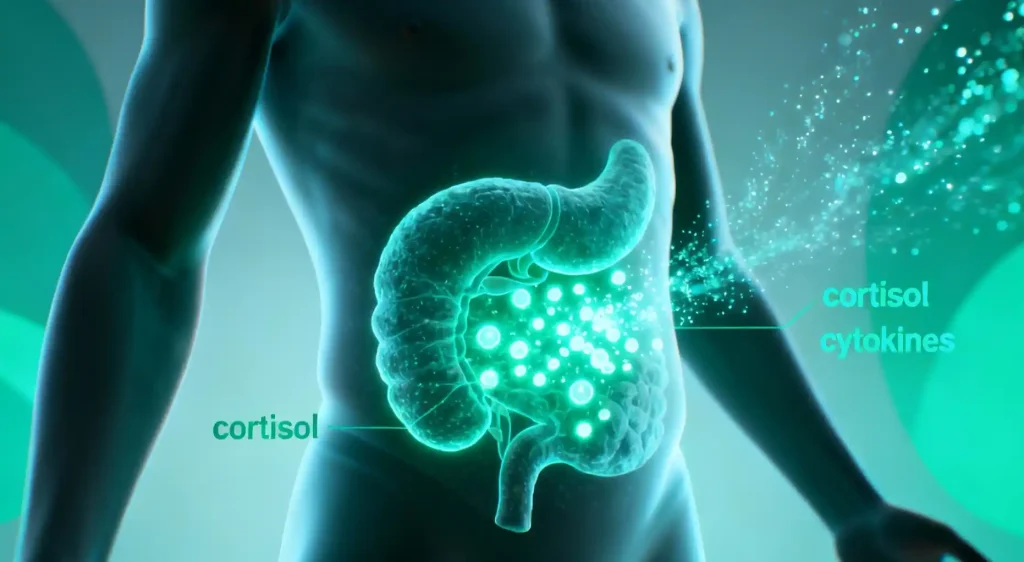
Cytokine Release: Visceral fat releases inflammatory markers called cytokines, which contribute to systemic inflammation (“inflammaging”).
Cortisol Production: Shockingly, visceral fat contains an enzyme (11-beta HSD1) that can convert inactive cortisone back into active cortisol.
The Vicious Cycle: This means belly fat can produce its own stress hormones, keeping local cortisol levels high even if blood levels drop, making it stubborn to lose.
2. Why Does Stress Specifically Target the Belly?
Stress specifically targets the belly because deep abdominal fat cells are biologically engineered to be sensitive to cortisol. These cells contain a significantly higher density of “glucocorticoid receptors” compared to subcutaneous fat (the fat on your arms or legs), making them the primary destination for fuel storage during times of perceived danger.
Receptor Density and Sensitivity
The distribution of fat in the human body is determined by receptor sites.
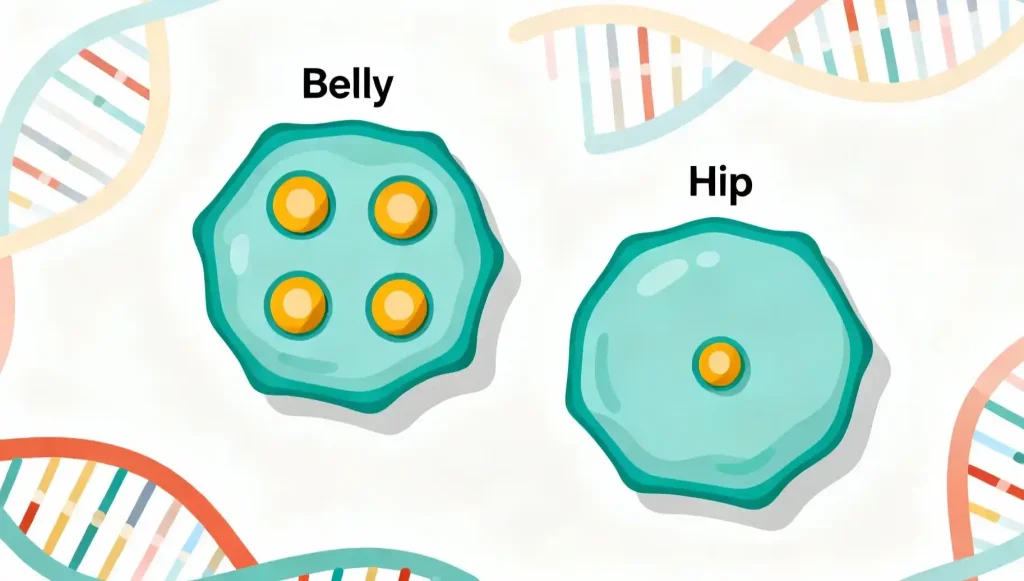
- The Magnet Effect: Think of cortisol receptors as docking stations. Because belly fat has roughly 4x more of these stations, cortisol “docks” there most frequently.
- Lipoprotein Lipase (LPL): Cortisol activates LPL, the enzyme responsible for fat accumulation, specifically in the central region.
- Subcutaneous Difference: Fat on the hips or thighs often responds more to estrogen or progesterone. Fat on the belly responds primarily to cortisol and insulin.
According to the The Obesity Society, abdominal obesity carries a higher metabolic risk than fat stored in other regions of the body.
The Evolutionary “Survival” Mechanism
From an evolutionary perspective, storing fat in the belly is a brilliant survival strategy.
- Quick Access: The abdomen is close to the liver. In a famine or long winter, the liver can quickly access these fat stores to convert them into energy.
- Protection: Visceral fat pads the vital organs (liver, pancreas, intestines) from physical trauma.
- Modern Mismatch: Our bodies equate “chronic work stress” with “impending famine.” The body holds onto belly fat as an insurance policy against starvation, unaware that the grocery store is full.
Reducing these false survival signals requires lowering daily mental stimulation adopting a digital minimalism lifestyle helps calm the nervous system and reduces stress-driven fat storage.
3. How Does Insulin Resistance Compound the Problem?
Insulin resistance compounds the problem because cortisol actively opposes insulin. When cortisol is chronically high, it renders cells resistant to insulin, forcing the pancreas to pump out more. High levels of insulin lock fat cells in “storage mode,” making it biochemically impossible to burn belly fat even with a calorie deficit.
The Cortisol-Insulin Loop
Cortisol and insulin have a complicated relationship. Cortisol raises blood sugar; insulin lowers it.
- Desensitization: When cortisol constantly floods the blood with glucose, the cells eventually stop listening to insulin’s signal to absorb it.
- Hyperinsulinemia: The pancreas compensates by producing massive amounts of insulin to force the sugar into cells.
- The Storage Lock: Insulin is a storage hormone. When insulin is high, lipolysis (fat burning) is blocked. You end up with high blood sugar and high fat storage simultaneously.
Chronic overstimulation worsens this loop by driving reward-seeking and sugar cravings understanding the real dopamine detox benefits can help break this stress-eating cycle.
Gluconeogenesis
This is the process where the liver creates new glucose.
- Muscle Breakdown: High cortisol triggers the breakdown of muscle tissue to get amino acids, which the liver converts into glucose (gluconeogenesis).
- Double Whammy: You lose metabolically active muscle mass (lowering your metabolism) and gain blood sugar (increasing fat storage).
- The Result: This leads to the “skinny fat” physique thin arms and legs (due to muscle wasting) and a protruding belly (due to fat deposition).
4. Why Does Sleep Deprivation Worsen the Cycle?
Sleep deprivation worsens the cycle because it disrupts the natural circadian rhythm of cortisol. Normally, cortisol should be low in the evening and high in the morning. Lack of sleep keeps cortisol elevated at night and disrupts the hunger hormones ghrelin and leptin, leading to intense cravings for high-sugar foods that fuel belly fat.
Elevated Evening Cortisol
A healthy cortisol curve follows the sun: high at 8 AM, low at 10 PM.
- The “Tired but Wired” State: If you don’t sleep well, the HPA axis becomes hyperactive. You get a spike of cortisol in the evening, preventing deep sleep.
- Growth Hormone Suppression: As discussed in previous articles, Growth Hormone helps burn fat and build muscle. High evening cortisol blocks the release of Growth Hormone, which normally occurs during deep sleep.
- Insulin Sensitivity Drop: Even one night of partial sleep deprivation can reduce insulin sensitivity by up to 30% the next day, priming your body to store your breakfast as fat.
Ghrelin and Cravings
Sleep regulates appetite.
- Ghrelin Spike: Sleep loss increases ghrelin (the “I’m hungry” hormone).
- Leptin Crash: It decreases leptin (the “I’m full” hormone).
- Hedonic Hunger: The brain specifically craves high-carb, high-fat foods because they provide a quick dopamine hit to a tired brain. These are exactly the foods that, when combined with high cortisol, are stored directly as visceral fat.
5. How Can You Lower Cortisol Naturally?
You can lower cortisol naturally by engaging the parasympathetic nervous system through low-intensity movement and psychological reframing. Unlike high-intensity exercise, which can spike cortisol, activities like walking, slow breathing, and nature exposure signal safety to the brain, allowing the HPA axis to downregulate.
Low-Intensity Movement (Zone 2)
High-Intensity Interval Training (HIIT) is popular, but for someone with high stress, it can be detrimental.
- The Cortisol Cap: Intense exercise creates a cortisol spike. If your baseline is already high, this adds fuel to the fire.
- Walking (Optical Flow): Walking while looking at the horizon creates “optical flow,” which quiets the amygdala (fear center).
- Zone 2 Cardio: Keeping your heart rate at a conversational pace increases blood flow and burns fat without triggering a “flight” response from the adrenals.
Psychological Reframing
Stress is often about perception.
- The physiological Sigh: As defined in previous toolkits, 2 inhales and 1 exhale manually slows the heart rate.
- Cognitive Distance: Viewing a stressful event as a “challenge” rather than a “threat” changes the hormonal response. A “challenge” releases adrenaline (energy); a “threat” releases cortisol (defeat/storage).
- Social Connection: Releasing oxytocin through hugging, pets, or conversation acts as a direct antidote to cortisol.
6. What Role Does Nutrition Play in Recovery?
Nutrition plays a recovery role by stabilizing blood sugar and providing the raw materials for adrenal function. Avoiding blood sugar crashes prevents the adrenal glands from releasing “emergency” cortisol, while nutrients like magnesium, Vitamin C, and Omega-3s help metabolize and clear stress hormones from the body.
Blood Sugar Stabilization
Every time your blood sugar crashes (hypoglycemia), the body releases cortisol to bring it back up.
- The Glucose Rollercoaster: A breakfast of cereal and juice causes a spike, then a crash. That crash triggers a cortisol release mid-morning.
- Savory Breakfast: Starting the day with protein and healthy fats (eggs, avocado) keeps glucose stable, keeping the cortisol “emergency brake” disengaged.
- Fiber Intake: Soluble fiber feeds healthy gut bacteria, which regulate the gut-brain axis and can lower systemic stress signals.
Nutrients for Adrenal Support
The adrenal glands consume specific nutrients at a high rate during stress.
- Vitamin C: The adrenal glands have the highest concentration of Vitamin C in the body. It is required to produce cortisol. Replenishing it helps regulate the cycle.
- Magnesium: Known as the “relaxation mineral,” magnesium dampens the HPA axis hyperactivity. Stress depletes magnesium, so supplementation is often necessary.
- Phosphatidylserine: An amino acid derivative found in fish and organ meats that has been shown to blunt the cortisol response to exercise and mental stress.
Stress Belly vs Regular Fat: How to Tell the Difference
This table helps you identify if your weight gain is hormonal or caloric.
| Feature | Stress Belly (Visceral Fat) | Regular Weight Gain (Subcutaneous) |
| Location | Protruding, firm belly; thin arms/legs. | Evenly distributed (hips, thighs, arms). |
| Texture | Hard and round (behind the muscle). | Soft and squishy (above the muscle). |
| Triggers | Sleep loss, anxiety, sugar crashes. | Excess calories, inactivity. |
| Risks | Heart disease, diabetes, inflammation. | Joint pressure, mobility issues. |
Practical Tools to Lower Cortisol and Release Belly Fat
To manage cortisol and belly fat, you need tools that signal safety to your nervous system.
1. The “Physiological Sigh” Protocol
- What it is: A specific breathing pattern: two sharp inhales through the nose (to fully inflate the sacs in the lungs), followed by one long, extended exhale through the mouth.
- Why it works: This is a mechanical “off switch” for the stress response. It offloads carbon dioxide and stimulates the Vagus nerve, slowing the heart rate within seconds. It is the fastest way to lower acute cortisol in real-time.
2. Morning Light Viewing (Circadian Reset)
- What it is: Getting outside for 10–20 minutes within the first hour of waking.
- Why it works: Sunlight hits the eyes and triggers a healthy morning cortisol spike (which is good!). This “timed” release ensures that cortisol drops later in the evening. If you miss the morning light, your cortisol curve flattens and drags out, leading to evening belly fat storage signals.
3. Adaptogenic Herbs (Ashwagandha/Rhodiola)
- What it is: Natural herbs that help the body “adapt” to stress.
- Why it works: Studies suggest these compounds can lower serum cortisol levels by up to 30%. They work by modulating the communication between the brain and the adrenal glands, preventing the “over-reaction” to daily stressors. Note: Always consult a doctor before starting supplements.
4. The “No-Phone” Walk
- What it is: A 20-minute walk without podcasts, music, or texting.
- Why it works: It combines “optical flow” (visual movement) with the absence of digital demands. This allows the brain to process thoughts (“background processing”) without new inputs, clearing the “cognitive cache” and lowering background anxiety.
Case Studies: Healing the Stress–Fat Loop
The “Healthy” Runner Mark, a 40-year-old executive, ran 5 miles every day and ate low-carb, yet he had a distinct “potbelly” that wouldn’t go away. He felt exhausted and relied on 4 coffees a day. After testing, his cortisol was found to be chronically high his intense running was actually adding to his work stress load. He switched from running to walking and heavy weight lifting (3x a week) and prioritized 8 hours of sleep. In 4 months, he lost 3 inches off his waist. He didn’t exercise more; he exercised smarter for his hormones.
The Postpartum Plateau Jessica couldn’t lose the “baby weight” two years after giving birth. She was barely eating, trying to starve the fat off, which only made her more anxious. She learned that caloric restriction is a form of stress. She started eating more (specifically protein and healthy fats) and focused on “Non-Sleep Deep Rest” (NSDR) during her toddler’s naps. By signaling safety through food abundance and rest, her body finally felt safe enough to release the stored energy. She lost 15 pounds by eating more and stressing less.
(Note: Names and identifying details have been adjusted to preserve privacy while maintaining biological accuracy)
A Simple Daily Cortisol Reset Routine:
If belly fat is driven by stress, your daily goal is simple: send safety signals repeatedly.
- Morning:
- 10–20 minutes of outdoor light
- Protein-based breakfast
- Midday:
- 10–30 minute walk (no phone)
- Avoid skipping meals
- Evening:
- No intense exercise
- Screens off 60 minutes before bed
- One calming ritual (stretching, breathing, reading)
Consistency matters more than intensity. The body releases fat only when it feels safe.
For deeper recovery, explore our guides on dopamine detox benefits, mental focus techniques, and simplifying digital life because fat loss begins in the nervous system, not the gym.
Frequently Asked Questions (FAQ):
Can I exercise away cortisol belly fat?
You cannot “crunch” it away. Ab exercises strengthen the muscle under the fat, but won’t burn the fat itself. The best exercise for cortisol management is a mix of low-intensity walking (to lower stress) and heavy resistance training (to build metabolic machinery). Avoid excessive cardio if you are already burned out.
How long does it take to reduce a cortisol belly?
It is slower than regular weight loss because you are fighting a survival mechanism. It typically takes 3–6 weeks of lifestyle changes (sleep, stress management) to lower the cortisol baseline before the body begins to release the visceral fat stores.
Does coffee make belly fat worse?
It can. Caffeine stimulates the adrenal glands to release cortisol. If you drink it on an empty stomach or when you are already stressed, it amplifies the fat-storage signal. Try drinking coffee after breakfast to mitigate the cortisol spike.
Is visceral fat dangerous?
Yes, it is the most dangerous type of fat. Because it surrounds organs like the liver and heart, it constantly pumps fatty acids and inflammatory cytokines into the bloodstream, increasing the risk of Type 2 diabetes and heart disease significantly more than hip or thigh fat.
Why do I crave sugar when I’m stressed?
This is a biological drive. Your brain wants “quick fuel” to fight the imaginary tiger. Sugar provides the fastest energy source. Additionally, sugar releases opioids and dopamine in the brain, temporarily numbing the feeling of stress a form of biological self-medication.
Final Verdict:
Having the connection between cortisol and belly fat explained reveals a critical truth: you cannot heal a body you are at war with. The stubborn fat around your midsection is not a sign of laziness; it is a sign of a body trying to protect you from a perceived threat. By shifting your focus from “burning calories” to “signaling safety” through sleep, nutrition, and calming movement you can turn off the alarm system. Once the body realizes the war is over, it will naturally release the reserves it was hoarding.
If stress is driving belly fat, it’s often part of a larger pattern involving sleep disruption, dopamine overload, and digital stress. Resetting cortisol works best when combined with nervous system regulation and attention recovery.